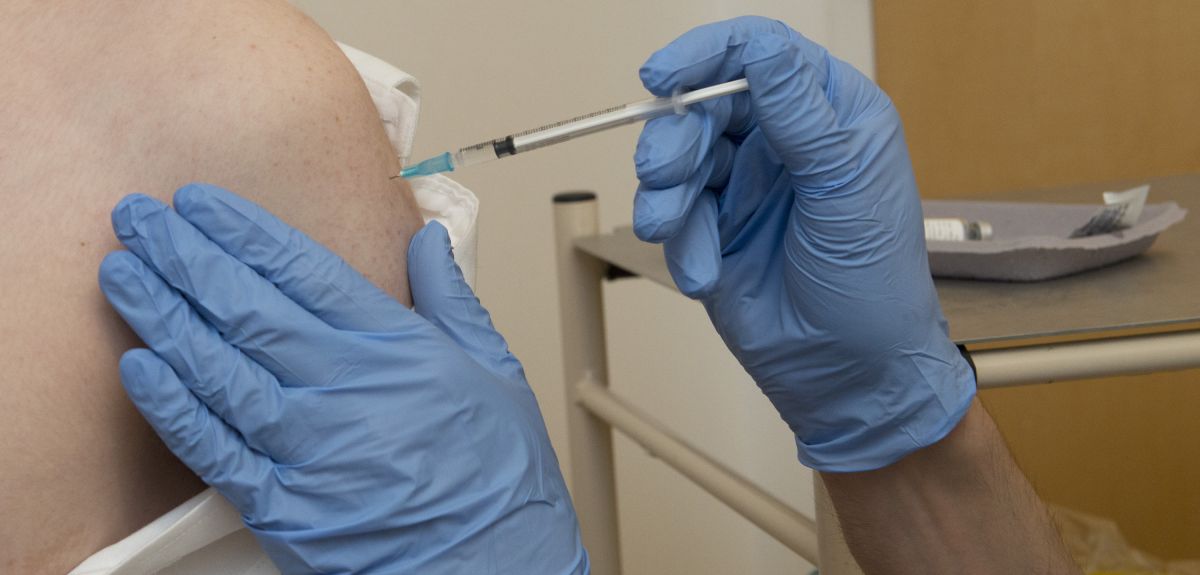
Credit: Oxford University Images
Booster Ebola vaccine enters first trials at Oxford University
Oxford University scientists have begun testing the safety of a candidate booster vaccine against Ebola, to find out whether it could further increase the immune responses seen in 30 healthy volunteers.
All the adult volunteers have previously received an experimental Ebola vaccine being developed by GSK and the US National Institutes of Health (NIH) as part of an ongoing trial at the Jenner Institute at Oxford University.
This was one of several safety trials of the GSK/NIH vaccine candidate – in the USA, UK, Mali and Switzerland – that were fast-tracked in response to the Ebola outbreak in West Africa, which has now claimed around 5,700 lives.
Initial results from a US trial in 20 people of a related Ebola vaccine formulation were published on Wed 26 Nov, and well over 200 people across the four sites have now received the candidate vaccine targeted for use in Africa. If the safety and immunogenicity data from the various trials are promising, the expectation is that the vaccine will move into much larger scale studies in West Africa, testing how effective the vaccine is.
If a single dose of an Ebola vaccine is sufficient, it makes absolute sense to use that. But it also makes sense at this early stage of trials to see if a second booster vaccine can greatly increase the levels of immune responses produced.
Professor Adrian Hill
The Oxford University trial saw 60 people vaccinated between 17 Sep and 18 Nov. Initial results are expected to be published before Christmas, although follow-up of the vaccinees will continue beyond those initial data.
30 of the volunteers are now being invited to receive a second candidate Ebola vaccine of a different type made by Bavarian Nordic, a company based in Denmark.
As neither vaccine contains infectious Ebola virus material, they cannot cause a person who is vaccinated to become infected with Ebola.
The new part of the Oxford trial continues to be funded under a grant from the Wellcome Trust, the Medical Research Council (MRC) and the UK Department for International Development (DFID).
The trial is testing the safety of the booster vaccine, given 3–10 weeks after the first, and will measure the immune responses seen in the volunteers over a period of 6 months.
Professor Adrian Hill, who is leading the trial at Oxford University's Jenner Institute, said: 'The aim of this trial is to tell us something about the safety of these two Ebola vaccines used in combination, and whether the second booster vaccine can increase immune responses further.
'If a single dose of an Ebola vaccine is sufficient, it makes absolute sense to use that. But it also makes sense at this early stage of trials to see if a second booster vaccine can greatly increase the levels of immune responses produced. There is real uncertainty about what level of vaccine-induced immunity is required to protect people against Ebola. The more data we have, the more we can make good decisions on what is likely to be safe, what may offer best chance of protection and what is feasible and achievable.
'We have seen promising results from the first 20 people vaccinated with a multi-strain formulation in the USA – the vaccine is well tolerated and does generate an immune response. How long that response lasts, and what level of immune response we need to offer people protection from Ebola we don’t know as yet. It is only larger trials in West Africa that will begin to tell us that.'
This approach using two vaccines is known as 'prime-boost'. It involves a first vaccination to stimulate, or 'prime', an initial immune response. A second vaccination given a few weeks later then 'boosts' the level of the body's immune response further.
The first 'prime' vaccine is the GSK/NIH Ebola vaccine, which uses a single Ebola virus gene in a chimpanzee adenovirus to generate an immune response. The gene comes from the Zaire species of Ebola, which is the one circulating in West Africa.
The second 'boost' vaccine from Bavarian Nordic uses the same Ebola virus gene in a modified vaccinia Ankara (MVA) virus.
The approach is not unusual – over 20 trials of experimental vaccines for malaria, hepatitis C, HIV, tuberculosis and flu have used prime-boost regimes with adenovirus- and MVA-based vaccines. In these cases, the boost vaccine was able to increase the immune responses seen substantially – around 30 fold for antibodies and 5–10 fold for T cells. Many of the people vaccinated were participating in malaria vaccine trials in Africa. Studies in monkeys in the USA showed that a prime-boost approach offered longer-lasting protection against Ebola. Though what immune responses will be found with these candidate Ebola vaccines in humans remains to be seen.
 Oxford University spinout Dark Blue Therapeutics acquired to advance leukaemia treatment
Oxford University spinout Dark Blue Therapeutics acquired to advance leukaemia treatment
 Expert Comment: Ethics-washing and Us-washing
Expert Comment: Ethics-washing and Us-washing
 GSK, University of Oxford and Imperial College London launch centre to create computer models of lungs, liver, kidneys and cartilage
GSK, University of Oxford and Imperial College London launch centre to create computer models of lungs, liver, kidneys and cartilage
 World Happiness Report 2026 shows a complex global picture of social media and happiness
World Happiness Report 2026 shows a complex global picture of social media and happiness
 Saïd Business School appoints first Poet Laureate
Saïd Business School appoints first Poet Laureate
 Trials of an experimental Ebola vaccine progress at speed
Trials of an experimental Ebola vaccine progress at speed
 First volunteer receives new Ebola vaccine in UK trial
First volunteer receives new Ebola vaccine in UK trial
 Oxford to lead trial of experimental drug in Ebola patients
Oxford to lead trial of experimental drug in Ebola patients