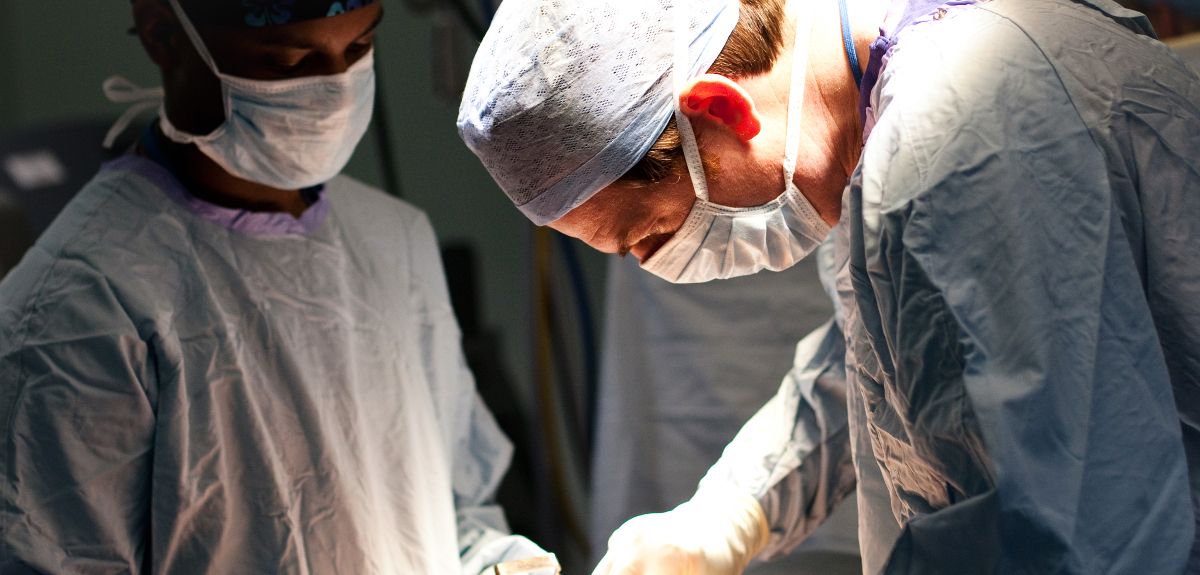
Image credit: Academy of Medical Sciences
Making patients safer in surgery
Surgery is getting safer thanks to research by an Oxford University team that has brought together two previously competing theories about how best to protect patients.
Previous attempts to improve patient safety in surgery used one of two approaches. Some investigators tried to improve teamwork and communication by training team members to interact better, using principles developed in the aviation industry. Others have focused on the systems of work and used industrial quality improvement techniques to rationalise these and remove or modify steps which carry a high risk of error.
It is not enough to just fix the system and it’s not enough to just train the team. You have to do both.
Professor Peter McCulloch, Nuffield Department of Surgical Sciences
A programme of studies, funded by the Programme Grants for Applied Research section of the National Institute for Health Research (NIHR), was carried out over four years by the Department of Surgical Sciences at Oxford University. It is believed to be the largest, direct observational study of surgical team performance during whole procedures ever completed.
The team ran five identical studies comparing the culture approach, two different systems approaches and two combined culture/system approaches. They found that the combined system/culture approaches were clearly better than either of the single approaches. This is an important idea which may change practice internationally.
Two new papers, published in the journal Annals of Surgery, outline the results of their research.
Professor Peter McCulloch, Principal Investigator of the project and head of the Quality, Reliability, Safety and Teamwork Unit (QRSTU), said: ‘One set of interventions tried to modify the culture of the team and the other tried to improve the system of work. No one had asked which of these was better, or whether combining the approaches would be more effective. It is not enough to just fix the system and it’s not enough to just train the team. You have to do both.’
In addition, the research showed that clinical staff who receive teamwork training become better motivated and more knowledgeable about safety risks, but are not able to change their working practices. Those who are helped to improve their system are able to do this, but are not educated or motivated to focus on the changes which will be most beneficial for patients. Staff who received the combined intervention developed more ambitious projects and demanded more help from the experts.
Lorna Flynn, Human Factors Research Assistant within QRSTU and first author of the second, qualitative paper, commented: ‘In addition to telling us that integrated approaches targeting systems and culture produce the best outcomes; our research has highlighted the fact that frontline staff do not have the time or means to address patient safety issues alone. Whilst frontline staff will possess local in-depth knowledge about their systems and working context, effective improvement work still requires substantial support from experts in the fields of Human Factors/Ergonomics and Quality Improvement. These findings have implications for practice in organisations where frontline clinical staff are often expected to do this work as part of their everyday clinical work; such an approach is not going to be sufficient in making significant change to patient safety unless healthcare organisations engage with experts in these fields.’
The papers, Combining systems and teamwork approaches to enhance the effectiveness of safety improvement interventions in surgery: the Safer Delivery of Surgical Services (S3) and The Safer Delivery of Surgical Services Programme (S3): explaining its differential effectiveness and exploring implications for improving quality in complex systems, are published in the journal Annals of Surgery.
 New study on Amazonia's fire crises urges action ahead of the next burning season
New study on Amazonia's fire crises urges action ahead of the next burning season
 New heart disease calculator could save lives by identifying high-risk patients missed by current tools
New heart disease calculator could save lives by identifying high-risk patients missed by current tools
 Modern Slavery and Human Rights Policy and Evidence Centre moves to Oxford University after receiving continuation funding
Modern Slavery and Human Rights Policy and Evidence Centre moves to Oxford University after receiving continuation funding
 Study shows that island bats are valuable allies for farmers
Study shows that island bats are valuable allies for farmers
 Study reveals how humanity could unite to address global challenges
Study reveals how humanity could unite to address global challenges